(below: the Tree of Life painting filled with survivors’ signatures located at Duke Women’s Cancer Center Macon Pond)

When my children were young our family spent a great deal of time playing in the back yard and relaxing on the porch swing. One of these lazy afternoons when I decided it was time for the children to go inside and complete some procrastinated chores, my youngest tried to sway my decision to let her stay out longer by saying she was trying to have “a beautiful moment.” Although her tactic didn’t get them out of chores, it did create a phrase commonly used in our family from then on. “A beautiful moment” became code family language for “that one perfect moment when all is well with the world.” Through the years when we were surrounded by loved ones blowing out birthday candles or if we were exhausted at the end of a long, hard day and heard our children laughing upstairs, I would whisper to my husband, “Shh. Listen. It’s a beautiful moment.”
Ringing the Bell
Celebrating “a beautiful moment” doesn’t mean life is without conflict. On the contrary, this mindfulness can come in the midst of a great battle to mark a time of peace and celebration. For instance, our family, like countless others facing cancer, had a monumental day we will never forget when I finished 17 Herceptin infusions and rang the treatment completion bell at Duke Women’s Cancer Center. Thankfully, I am not alone with this milestone. According to The American Cancer Society, 85% of those diagnosed with Breast Cancer in 2022 will survive and reach the cancer completion bell due to early detection and treatments options.
(below: Surrounded by chemo nurses as I completed my 17th infusion and rang the bell May, 2021)


My First Cancerversary
Soon after ringing the cancer bell, I celebrated my cancerversary, which is the date that cancer survivors consider themselves cancer free. My cancerversary is June 2, the date that I had a double mastectomy removing all cancer from my body. While survivors all celebrate a cancerversary differently, it was cathartic for me on my first cancerversary to spring clean my medicine cabinet, tossing out empty medicine bottles that I had used to manage the adverse effects of chemotherapy. I also marked the achievement by donating the scarves that had covered my bald head to my cancer center for fellow patients who might need them. In fact, some of the scarves I donated were given to me by friends of friends who I have never even met because when breast cancer survivors hear about a new diagnosis they feel a kindred connection, often reaching out to help one another cope with the life-changing diagnosis. It felt like I was channeling some strength from these brave women who had walked the same path before me.


Port-A-Cath Removal
Like many people I have always been squeamish about needles in general, so one of my many fears about breast cancer was whether infusions would be painful. I pictured nurses struggling to find a vein in my arm, and I couldn’t imagine sitting with a needle in my arm for hours. Thankfully, administering chemo treatment has advanced greatly with the invention of the port-a cath. A port-a-cath, or chemo port as many refer to it, is a small plastic device inserted just below the skin that connects to a major vein so that health care workers can draw blood and administer infusions easily and painlessly. It truly makes the experience so much easier because patients put a little numbing cream on the area of skin an hour before the doctor’s appointment and honestly feel no pain during infusion. I highly advise it for anyone anticipating several treatments like I had. At the end of treatment, the port-a-cath is removed during out-patient surgery and a tiny scar is left behind as a badge of courage.



A Little Body Fat and Some Silicone
After a year of having hard plastic expanders in my chest, another “beautiful moment” on my cancer journey came when it was time to exchange extenders for implants during reconstructive surgery. For months my plastic surgeon used extenders to expand my chest area until I reached my previous breast size. Luckily, I did not find the expansion particularly painful although my right breast, which had undergone three previous lumpectomies and sixteen radiation treatments, was sorer than the left side since it had been stretched more during the process.
Breast reconstructive surgery involves a great deal of research and decision-making. Unlike breast enhancement surgery, reconstruction requires creating breasts from scratch since there is a bare chest cavity with no fat, muscle, nerves, or often nipples. The patient chooses either saline or silicone implants, and many women today choose to add fat grafting around the implants so that implants have a more natural shape. One method, known as the DIEP Flap, takes fat from the abdomen or thighs and transfers it to the breast so that the patient gets a tummy tuck along with breast reconstruction. It is a serious procedure, and patients are in the ICU for a few days before going home to a healing process that lasts for months. Although I’ve heard many success stories about the DIEP Flap, I wanted the fastest healing process, so I chose implants with fat grafting. As a result, the basis of my breasts are implants, but the surgeon used liposuction from my sides and hips to transfer fat to the breast area for contour. It is miraculous what surgeons can do today.
My only advice is if the patient has a low Neutrophil count, there is an infusion that boosts leukocytes (white blood cells) to safeguard patients from infections which can develop during and post surgery. Unfortunately, the oncologist must advocate for the infusion, which I found when my oncologist and my cancer center had to call the insurance three times to request it, but it made all the difference in successful healing after surgery.
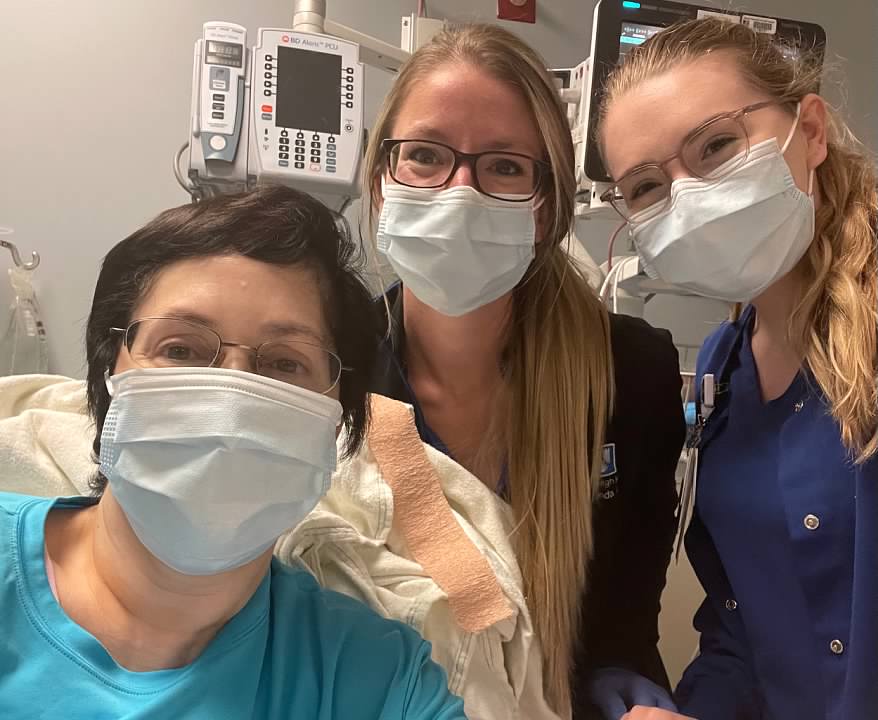
(below, nurses comforting me before reconstructive surgery since my husband could not be there due to COVID-19 restrictions)
Never Say “Never”
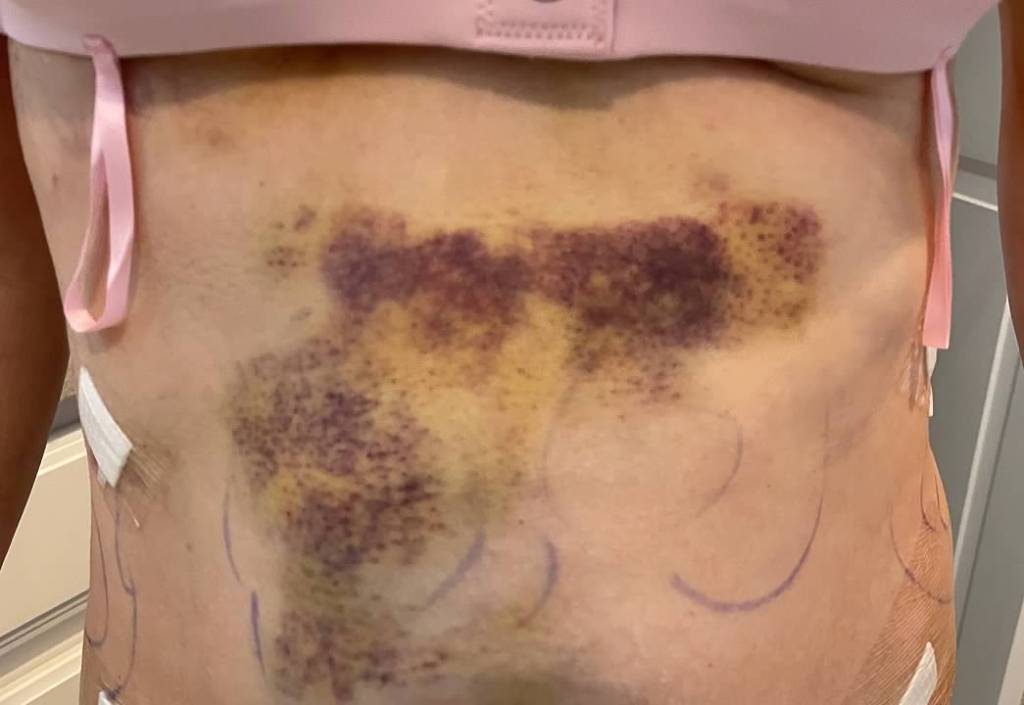
I never planned to have liposuction, breast enhancement surgery, or even a tattoo. However, as the saying goes, “Never say never,” because this year I received all three as part of my reconstruction process. The photo below shows where the surgeon used liposuction for fat grafting. The binder in the photo was worn continuously for six weeks, and I had to sleep on my back until cleared by my surgeon to sleep on my side again. I found a u-shaped full body maternity pillow very helpful to keep me in place while still cushioning my bruised sides so I could rest better. Overall, it takes approximately three months before all the bruising and swelling dissipate, but for most survivors there is little complaining because it feels more natural having saline or silicone in the breast area rather than hard plastic expanders.


Unfortunately, survivors who undergo radiation during cancer treatment can have more complications recovering from reconstructive surgery. I had sixteen radiation treatments which caused the radiated breast to heal differently from the non-radiated breast. For instance, a radiated breast is more likely to absorb fat from the grafting process, making it a little smaller than the other breast. The radiated breast can also develop capsular contracture, which causes painful tightness and difficulty moving the arm. As a result, some patients request further surgeries to relieve the pain and tightness. Although I developed capsular contracture, I am hoping the physical therapy I am doing will alleviate the tightness, Lymphedema, and flexibility on my right breast and arm. So far it is helping, so I am hopeful and marvel at the scientific advancements that allowed me a full, successful reconstruction.
A Spring Break Tattoo
Each step of the reconstruction process, like the cancer journey itself, is unique for each patient. For instance, after cancer treatment some patients decide against breast reconstruction completely, while others like me jump right into the reconstruction process. Therefore, no two journeys are exactly alike even for survivors with the same diagnosis.
During chemotherapy, I read, Pretty Sick, by Caitlin Kernan, a beauty editor who became a breast cancer survivor, and it made quite an impression on me. It introduced me to Vinnie Myers, and I researched the 3D tattoos he creates to help women look more like they did before mastectomies. Having received national acclaim on the Today Show, The Washington Post, The New York Times, among numerous other media outlets, Vinnie only creates 3D nipple tattoos and estimates to have completed approximately 13,000 3D tattoos for breast cancer survivors. Although not covered by insurance, I dreamed of having him complete the finishing touch because his work looked incredibly realistic, so I decided the $800 for two tattoos was worth the money.
After a little planning and waiting six months after reconstructive surgery, which is the time it takes to heal before a tattoo, I headed to Baltimore on my spring break for a weekend away with my husband, ending in two spring break tattoos at Vinnie’s Finksburg location.

Since it was my first tattoo, I wasn’t sure what to expect, and there is no consultation in advance. However, I the map on his office wall for patients to pinpoint their homes displayed that patients had traveled from every US state as well as every continent, which gave me confidence to relax and let Vinnie do his magic. The procedure itself, which took about an hour, was sensitive at times although many survivors claim to have no sensitivity at all. While he worked, matching ink colors to my skin tone, he entertained my husband and I with stories of the Grateful Dead and other celebrities he has known through the years. Afterwards, It felt like I had completed the final step in helping me feel healed, whole, and feminine again.
Body Dysmorphia is finally becoming a hot topic in the medical community for a good reason. Breast cancer survivors often lose body parts that they never imagined having removed, making many of them feel unattractive or incomplete afterwards. For many survivors the reconstructive surgery itself provides a feeling of closure, but for me it did not come until I completed the tattooing. Although my mastectomy scars remain, I no longer see them when I look at myself. Instead, I see the incredibly realistic tattoos, and I cannot emphasize how healing it has been for me. I fully understand that my choices are not for everyone, but I wanted to share my experience for any fellow survivor interested in this post-reconstruction option. I was always a woman despite having a mastectomy, but now I feel more like the person I was prior to my cancer experience.
The Road to Peace
Despite these beautiful moments and my grateful remission status, I still have periods of darkness when my anxiety feels overwhelming. For example, when a fellow survivor has a recurrence, my own fears flood back. Doctor appointments still give me PTSD as well, and any time I need a body scan I am restless until I receive good results. I also worry about every herb I take. For instance, I am a triple positive (ER+, PR+, HER2+) breast cancer survivor, meaning hormones rather than food or environment fueled my type of cancer, so while hormone replacement is popular today, I do the opposite and take aromatase inhibitors. Herbs and vitamins must also be monitored carefully, which can be challenging. For instance, I took collagen to help my hair grow and to strengthen my joints after chemotherapy but recently found research suggesting triple positive survivors might need to avoid it. Likewise, I took a multi-vitamin that I just discovered contained herbs that may accelerate female hormones. At present, I am seeking advice from my Duke support team to determine what vitamins and herbs are safe for me. Thankfully, I also have a support group led by Jen Hoverstad, a survivor and motivational speaker, and a dear friend, Joanna Rose, who has the same diagnosis as I do, so we help each other navigate these murky waters.
Although cancer survivors are living much longer lives, patients still need essential treatments and cures for so many types of cancer. If science can create a COVID-19 vaccine within months, I know we could could cure cancer with the necessary funding and urgency. At a time when many are cheering on Elon Musk’s SpaceX, I am frustrated, thinking what the cost of a 55 million dollar joyride to outer space could do for cancer research. My hope is that one day cancer treatment will become an urgent global research priority like the COVID vaccine was and that treatments like chemotherapy will be considered as outdated as a lobotomies.
Ironically, I never felt sick until I went through cancer, but at least this experience has made me appreciate each day to the fullest. Since cancer, I am trying to redirect my mindset to become as positive as I can for my own mental and physical wellbeing. It is essential for each survivor to find a beacon through the darkness, whether it be counseling, medication, meditation, or prayer.
Until we reach a cure, I hold firmly to a scripture I ran across one sleepless night: Hebrews 11:1: ” Faith is the confidence in what we hope for, the assurance in what we cannot see.” I literally recite this verse every day as my mantra. My hope for a cancer cure remains strong, but until then I, like my fellow survivors, continue to celebrate life’s beautiful moments, whether they be great or whether they be small.
*Opinions in this blog are my own.
“A Beautiful Moment” is dedicated to Cullen, Michael, and Elizabeth for giving me the most beautiful moments of my life.





This is fantastic! You and your family will remain in my prayers!
Charles
LikeLike
Thank you so much!
LikeLike
You are my hero! Thanks for sharing your story to help other sisters!
LikeLike
Ahhhh Ela, your post gives me such satisfaction! It has been a long road, but wow, you have reached the other side. You are still researching the best ways to help your body and mind continue healing. In short, you’re doing everything right! What an inspiration you are, meeting every challenge with grace and wisdom, relying on God’s grace as well. And I know how much you have relied on Cullen, Michael and Elizabeth for support, encouragement and unconditional love. You couldn’t have a better team at your side. So many of us will be eventually diagnosed with breast or another cancer. You give us hope that there can be abundant life beyond diagnosis and treatment. May God continue to hold you in the palm of his hand. I love you and am so happy for you right now.
Susan ❤️ xxxooo
>
LikeLike
Thank you so much for such a beautiful response! You give me strength and inspiration! Much love to you!
LikeLike